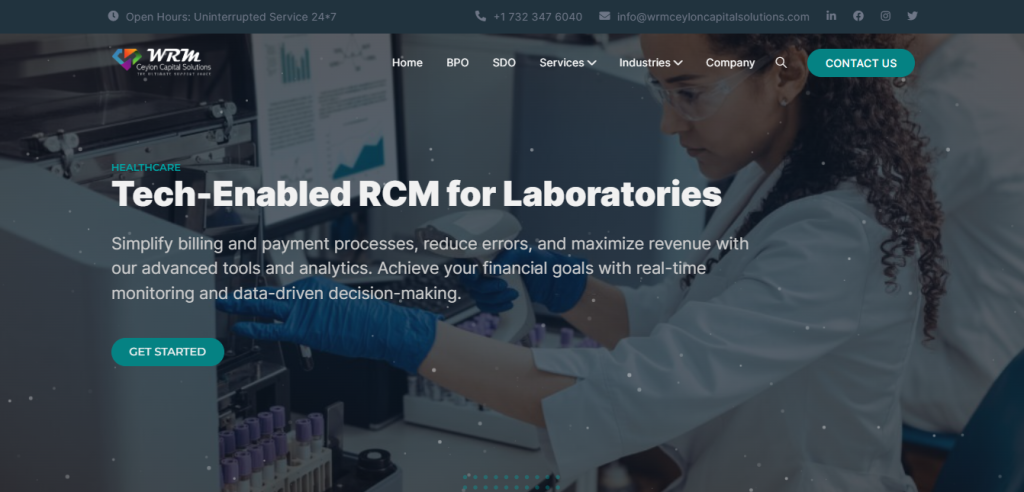
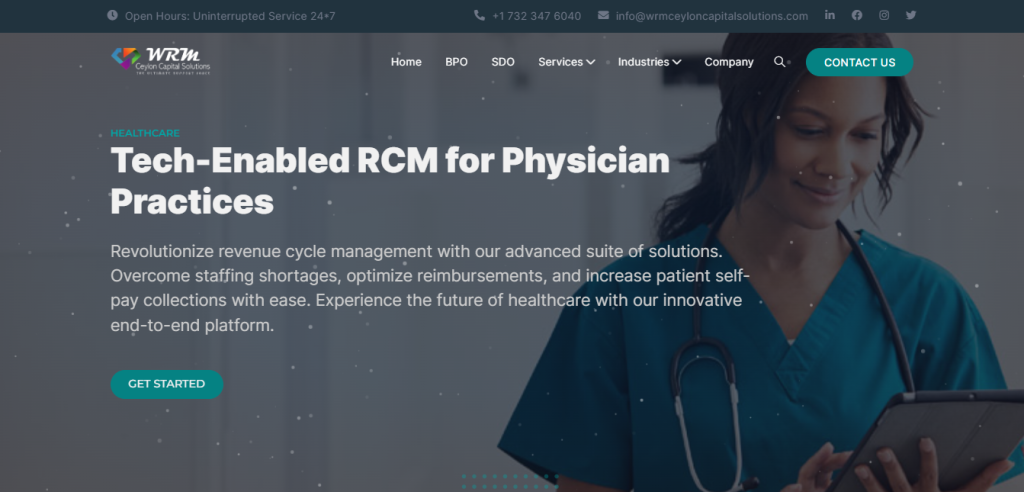
Let us be your partner in success. With our commitment to your organization’s growth and our tech-savvy solutions, we’re confident that we can help you achieve your goals and take your healthcare organization to new heights.
Don’t wait to transform your business – contact us today and start your journey to success.
Support success with outsourcing functions
Boost your revenue cycle operations by focusing on improving your accounts receivable (A/R), particularly the aging A/R and A/R workdown on older systems. To achieve this, ensure that you have the necessary skills and resources to optimize your revenue cycle functions.

Partner with the experts
We provide top-notch account management services that give you direct access to a reliable and dedicated point of contact. Our team offers in-depth analysis and valuable insights to help you turn raw data into practical and actionable steps that can transform your business.

Get visibility into the reimbursement cycle
With our services, your organization can gain real-time access to cutting-edge analytics and leverage our expertise to make the most of your technology. And the best part? You’ll still maintain full control of your finances.

Streamline billing workflows
Our solution includes a comprehensive, rules-based engine that automates tasks, simplifies workflows, and enhances cash flow.

Identify issues and improve performance
Our approach is proactive and focuses on identifying the root cause of issues to prevent them from recurring in the future. We help you hold departments accountable for their performance and take necessary steps to ensure that your operations run smoothly.
Improved reporting and analytics
We offer transparent reporting of your revenue cycle results and metrics, including valuable analytics to help you optimize insurance and self-pay collections.

Revenue Cycle Analytics & Performance Management
Make data-driven decisions with revenue cycle analytics insights
Our exclusive analytic toolset provides exclusive insights into the revenue cycle, allowing you to identify trends and make informed decisions that improve your financial outcomes. Our technology monitors critical factors like physician productivity, denial trends, and industry benchmarks, providing transparency into the revenue cycle.
Effective collections processes and best practices
Our approach covers the complete revenue cycle continuum, from operational planning and scheduling to final collections and reporting.
Professional billing experts
We work closely with you to ensure accurate billing and coding and support you at every stage of the revenue cycle. Our dedicated account managers provide a comprehensive approach to enhance the financial health of your practice.

Transform the operator experience
Our tools empower revenue cycle operators to focus on strategic tasks, improve performance, reduce denials, and optimize collections. Real-time data and analytics identify trends and issues, while automation and workflow tools streamline processes, reducing manual errors and improving cash flow. Our ultimate goal is to drive revenue and improve financial health for healthcare organizations.
Resource Augmentation
Resource Augmentation services can help companies to improve their operational efficiency, reduce costs, and accelerate their business growth.
Increased flexibility: Companies can quickly and easily scale their workforce up or down based on their changing needs, without the long-term commitment of hiring permanent employees.
Access to specialized skills: Companies can access a pool of specialized skills and expertise that may not be available within their organization, without the cost of recruiting and training new employees.
Cost-effectiveness: Resource Augmentation services can be a cost-effective solution compared to hiring permanent employees, as companies only pay for the resources they need for a specific project or period.
Reduced time-to-hire: Companies can quickly fill skill or resource gaps without the time-consuming process of recruiting and onboarding new employees.

Revenue Cycle Automation
RCA can help healthcare organizations to improve their revenue cycle performance, reduce costs, and provide a better patient experience.
Increased efficiency: By automating manual processes, RCA can significantly reduce the time and effort required to manage revenue cycle processes. This can help to improve productivity and reduce operational costs.
Improved accuracy: RCA can help to reduce errors and inaccuracies that can occur in manual processes. This can help to improve data quality, reduce claim denials, and improve overall revenue cycle performance.
Faster payment processing: By automating claims submission and payment processing, RCA can help to speed up the payment process and reduce the time it takes to receive payment for services rendered.
Improved patient experience: RCA can help to improve the patient experience by streamlining the registration and payment process, reducing wait times, and improving the accuracy of billing and payment information.

Credentialing Services
Credentialing is the process of verifying the qualifications, experience, and professional standing of healthcare providers to ensure that they meet the standards set by insurance payers. Credentialing services help healthcare providers navigate this process by managing the application, verification, and approval process for individual providers and organizations. Some of the key activities involved in credentialing services include:
- Collecting and verifying provider credentials, including licenses, certifications, and education.
- Submitting applications to insurance payers for credentialing and re-credentialing.
- Tracking the status of applications and following up with insurance payers as needed.
- Maintaining accurate records of provider credentials and renewals.

Payer Management Services
Helps healthcare providers to manage their relationships with insurance payers, including negotiating contracts, submitting claims, and managing payments. These services are designed to help providers optimize revenue collection, reduce administrative costs, and improve patient satisfaction. Some of the key activities involved in payer management services include:
- Negotiating payer contracts and fee schedules.
- Submitting and tracking insurance claims, including managing denials and appeals.
- Managing payment processing and collections.
- Monitoring payer performance and identifying opportunities for improvement.
Healthcare IT Services
Healthcare IT services cover care delivery digitalization, IT modernization, cloud migration, IT support, etc. We offers full-cycle IT services for medical organizations to leverage tech-enabled healthcare without expanding an in-house IT team.
We provide the following services separately or in combination.
Healthcare software development
- We provide healthcare solutions that are centered around patients, and involve administrative and care-related tasks.
- Our expertise includes developing software for medical devices, laboratory, medical imaging, and SaMD.
- We can deliver an MVP in just 2-4 months.
- Our solutions seamlessly integrate with healthcare IT systems, as well as medical devices and wearables.

IT modernization
- We specialize in integrating various healthcare applications such as EHR, medical imaging software, and practice management software.
- Our services also include modernizing legacy healthcare applications through recoding, reengineering, containerization, and other techniques.
- We can assist in consolidating data from different healthcare organizations and patients, to provide a unified view.
Cloud migration
- We help in selecting a HIPAA-compliant cloud for your healthcare organization to ensure security and compliance with regulations.
- Our cloud migration strategy considers cost-efficiency to optimize your spending.
- Our step-by-step migration approach involves breaking down applications into modules, making it easier to migrate them incrementally.
- Our services also include server, data warehouse, and desktop migration to ensure a smooth transition to the cloud.

Healthcare data analytics and performance management
- We specialize in designing and implementing analytics solutions for healthcare organizations.
- Our solutions enable patient outcomes analytics to identify trends and adjust treatment plans.
- We can also analyze patient-generated health data such as glucose levels, body temperature, weight, and blood pressure.
- Our services include performance evaluation and efficiency analysis of internal processes such as equipment utilization and bed allocation.
- We can provide financial management solutions such as analyzing expenses per episode, expected cash flow, and outstanding payments.
Benefits of Cooperation with Cey Cap Solutions

No need for large upfront investments
We follow an iterative approach that allows us to implement the initial improvements to your IT infrastructure or deliver the first version of your digital health solution within a short timeframe of 1-3 months.

Services tailored to your needs
We offer a range of healthcare IT services that you can choose from individually, or you can combine them to create a customized service pack that meets your organization's unique needs and covers all your healthcare processes.

Smooth collaboration
We establish efficient collaboration with all of our customers' stakeholders, self-manage our work, and are always ready to share our expertise. With us, you'll be fully informed about the project status as our cooperation is based on a pre-agreed process and a set of KPIs.
Healthcare IT Service Investments
- Complexity and depth of the project
- Type of technology used (e.g., software or hardware)
- Scope of the project
- Level of expertise required
- Degree of customization needed for the solution
- Type and complexity of the healthcare IT infrastructure (cloud or on-premises)
- Scope of modernization and digitalization needs (e.g., telehealth applications or digital therapeutics software)
- Level of support required (e.g., time coverage and number of tickets per month)
- Service-level objectives (e.g., uptime or response time)
All of these factors can influence the cost of healthcare IT services. It is important to have a thorough understanding of these factors to provide an accurate pricing estimate for healthcare IT services.
Doubt Healthcare IT Investments Will Pay Off?
At Cey Cap Solutions, we offer an iterative approach that allows our clients to start with smaller improvements and build upon them as they see results. This approach helps our clients to assess the impact of the changes made to their healthcare organization’s processes and decide on the next steps accordingly. By breaking down complex projects into smaller, manageable parts, we can achieve better results and ensure that our clients are satisfied every step of the way.
Optimize. Every stage of revenue cycle management.
As the healthcare industry continues to evolve, you want a partner that cares for your business the way you care for patients. We are uniquely positioned to help you anticipate the next normal.

Technology-Enabled Solutions
Integrating our healthcare IT solutions with your existing systems can lead to a more seamless patient experience and improved financial performance for your organization. By leveraging our tools and expertise, we can help you optimize processes, reduce errors, and increase efficiency. This can result in improved patient satisfaction, increased revenue, and reduced costs. Our goal is to work with you to create a comprehensive solution that meets your unique needs and delivers measurable results.

Intelligent Process Automation
We can help transform your business model by implementing digital solutions that streamline processes, increase productivity, and reduce operational risk. Our team can work with you to identify pain points in your current workflow and develop customized solutions to address them. By leveraging the latest technology, we can optimize your operations, improve efficiency, and reduce costs, leading to a more sustainable and profitable business model.

Deep Domain Expertise
At Cey Cap Solutions, we provide guidance to healthcare organizations to apply industry best practices that solve problems and create lasting value. Our team of experts has years of experience in healthcare IT and revenue cycle management and can help identify areas for improvement, develop solutions, and implement them in a way that maximizes their impact. By partnering with us, healthcare organizations can transform their operations, improve patient experience, and drive financial performance.

Cloud BI Development
We utilize container architecture to develop lightweight cloud-based applications. We prioritize industry compliance, governance, and security protocols and ensure that they are seamlessly integrated into all the Business Intelligence (BI) technologies we create.

BI Reporting & Dashboards
We specialize in creating powerful and flexible dashboards that feature reporting and analytics tools capable of delivering real-time insights through a range of pixel-perfect displays. Our dashboards and reporting tools are designed to be fully customizable and can operate on any browser or platform.

Data Science & Machine Learning
Our team has expertise in engineering advanced data science and machine learning tools that allow for data configuration and the creation of predictive models that can be customized and shared. Our machine learning models are capable of being automatically trained based on the data, ensuring accurate and reliable results.
Verification of Benefits (VBO) is a crucial process for healthcare providers to verify a patient’s insurance coverage and benefits before providing medical services. This helps both parties understand the extent of insurance coverage and the patient’s financial responsibility, avoiding unexpected medical bills. VBO empowers patients to make informed decisions about their healthcare, leading to better outcomes and experiences.
Medical billing is the process of submitting and following up on claims with health insurance companies to receive payment for medical services provided. It’s a critical component of healthcare revenue cycle management that ensures providers get paid for their services, while patients and insurance companies are charged accurately. Accurate medical billing is essential to streamline the payment process, prevent errors, and maintain a stable cash flow for healthcare providers.
Payment and denials posting is a crucial part of the medical billing process, where healthcare providers record and track payments received from insurance companies for medical services provided, as well as any claims that are denied. By accurately posting payments and denials, providers can ensure that they receive timely and appropriate reimbursement for their services, identify any issues with insurance claims, and take necessary steps to address and resolve them. Effective payment and denials posting can help providers streamline their revenue cycle management, reduce the risk of lost revenue, and improve overall financial performance.
Denial management is the process of identifying, analyzing, and resolving insurance claim denials to ensure that healthcare providers receive appropriate reimbursement for the medical services they provide. Denial management involves several steps, including identifying the root cause of the denial, appealing the claim, and correcting any errors or omissions in the billing process. Effective denial management can help healthcare providers reduce claim denials, optimize revenue cycle management, and minimize the risk of lost revenue. By streamlining the denial management process, providers can improve their financial performance, enhance patient satisfaction, and maintain a healthy cash flow.
Account Receivable (AR) Management is a crucial process for healthcare providers to effectively manage and collect outstanding balances owed by patients and insurance companies for medical services provided. AR Management involves tracking and monitoring outstanding invoices, following up with patients and insurance companies for payments, and resolving any issues that may arise. By implementing an effective AR management process, healthcare providers can reduce the risk of lost revenue, improve cash flow, and enhance overall financial performance. AR management also helps to maintain positive patient relationships and provide a better patient experience by addressing billing issues and concerns in a timely and efficient manner.
Revenue Cycle Analytics is the process of analyzing healthcare revenue cycle data to optimize financial performance and improve the patient experience. By identifying inefficiencies and trends, providers can make informed decisions, implement process improvements, and achieve better patient outcomes. Revenue Cycle Analytics helps healthcare providers reduce billing errors, enhance patient satisfaction, and improve financial performance.
Patient billing is a crucial process for healthcare providers to ensure accurate and timely payment for medical services provided. It involves clear statements, flexible payment options, and easy-to-understand explanations of insurance coverage and financial responsibility. By optimizing the patient billing process, providers can reduce errors, improve revenue cycle management, and enhance patient satisfaction. Effective patient billing helps providers maintain a healthy cash flow and build positive patient relationships.
Unleashing the Future of Development:
Discover Our Revolutionary Solutions
Read more . . .
Read more . . .
What Happens Next?
Our sales manager will contact you within a few days of analyzing your business requirements.
In the meantime, we will ask you to sign a non-disclosure agreement (NDA) to ensure the highest level of privacy.
Our pre-sale manager will present you with project estimates and an approximate timeline.